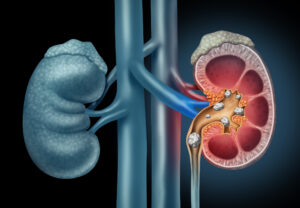
 Kidney stones are solid masses or clusters of crystals that form from substances such as minerals, acids, and salts in the kidneys. These stones can be as small as a grain of sand, or in rare cases, larger than a golf ball.
Kidney stones are solid masses or clusters of crystals that form from substances such as minerals, acids, and salts in the kidneys. These stones can be as small as a grain of sand, or in rare cases, larger than a golf ball.
Kidney stones occur when there is little liquid and too many of the minerals, acids, and other substances, such as calcium, sodium, oxalate, and uric acid, in the urine, causing them to stick together and form crystals or stones. Kidney stones can form over months or years.
There are four types of kidney stones, and they are named after the kind of crystal that they are made from. They include:
- Calcium-oxalate and calcium phosphate stones are the most common types of kidney stones
- Uric acid stones
- Struvite stones
- Cystine stones
Depending on the size of kidney stones, a person may not even realize that they have them. Smaller-sized stones can pass through the urinary tract in the urine without symptoms. However, larger-sized kidney stones can get trapped in the ureter, the tube that drains urine from the kidney down to the bladder, causing pee to back up and limit the kidney’s ability to filter waste from the body, which can also cause bleeding.
Kidney stones can take as long as three weeks to pass on their own. Sometimes, small stones can cause extreme pain as they go through the urinary tract and out of the body. If a kidney stone can’t pass on its own, a healthcare provider will need to break it up and remove it.
Kidney stones are common. About one in 10 people will get a kidney stone during their lifetime. They are most common in men who are in their 30s and 40s and among non-Hispanic white people.
The most common symptom of kidney stones is pain in the lower back, belly, or side, which might feel like it extends from the groin to the side. This pain can be dull, or it can be sharp and severe, and comes in waves. Other symptoms of kidney stones include:
- Bloody urine
- Pain when urinating
- The inability to urinate
- Feeling the urge to urinate a lot
- Cloudy or foul-smelling urine
- Nausea and vomiting
- Fever or chills
Several risk factors can cause someone to develop kidney stones, including:
- Not drinking enough fluids
- Eating foods high in sodium or sugars
- Eating meat and other protein-rich foods
- Having a family history of kidney stones
- Having a blockage in the urinary tract
- Taking vitamin C supplements
- Having had stomach or intestine surgery, including gastric bypass surgery
- Taking certain medications, such as diuretics, calcium-based antacids, and some antiseizure medications
- Having certain medical conditions, such as:
- Cystic fibrosis
- Diabetes
- Gout
- High blood pressure
- High levels of calcium in the urine
- Inflammatory bowel disease (IBD)
- Kidney cysts
- Obesity
- Osteoporosis
- Parathyroid disease
- Primary hyperoxaluria
- Hemiplegia or paraplegia, which are types of paralysis
Kidney stones can cause many complications, including:
- Chronic kidney disease (CKD)
- A blockage that backs up urine into the kidney, causing it to swell
- Acute kidney injury
- Kidney infection
- Frequent urinary tract infections (UTIs)
A healthcare provider can diagnose kidney stones by performing urine, imaging, and blood tests.
To treat a small kidney stone, a healthcare provider will have the person monitor their symptoms until the stone passes in their urine. They may also prescribe medications to keep them comfortable and help the stone pass on its own. Larger kidney stones need treatment depending on their size, location, whether they are causing infections or symptoms, and other factors.
Medications to treat kidney stones help relax the ureter to help pass the stone more easily, help manage any nausea and vomiting, and help manage pain.
Procedures to remove large kidney stones include:
- Shockwave lithotripsy
- Ureteroscopy
- Percutaneous nephrolithotomy
- Laparoscopic surgery
It is important to note that the things we eat and drink impact our risk for kidney stones. Talk to your healthcare provider or a dietitian about ways to reduce your risk of developing kidney stones. They may recommend:
- Drinking plenty of water
- Limiting consumption of foods high in sugar and sodium
- Limiting consumption of animal proteins
- Maintaining a weight that is healthy for you
- Eating foods that are good sources of calcium
- Limiting consumption of foods high in oxalates
- Prescription medications
If you are experiencing symptoms of kidney stones, and would like more information about receiving treatment from a urologist at Jamaica Hospital Medical Center. To make an appointment, please call 718-206-7001.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow







