 Everybody poops. That is a fact of life. Therefore, it is important to be aware of changes in your bowel movements, as they can indicate if there are potential health issues.
Everybody poops. That is a fact of life. Therefore, it is important to be aware of changes in your bowel movements, as they can indicate if there are potential health issues.
For example, hard, lumpy poop can mean you’re dehydrated. Red poop may be a sign of rectal bleeding. Pungent poop could indicate an infection or other concerns.
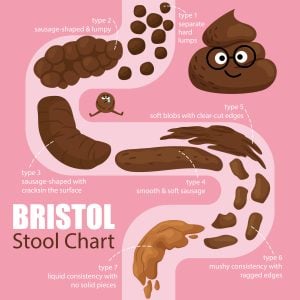
Some stools can be big or small depending on the day. It can be round or oblong. Or it can be hard, soft, or even liquid in form. The Bristol Stool Chart gives a sense of what’s ideal and what isn’t. It classifies stool into seven types based on shape and consistency. The types include:
- Type 1: Separate hard lumps, like little pebbles
- Type 2: Hard and lumpy and starting to resemble sausage
- Type 3: Sausage-shaped with cracks on the surface
- Type 4: Thinner and more snake-like, plus smooth and soft
- Type 5: Soft blobs with clear-cut edges
- Type 6: Fluffy, mushy pieces with ragged edges
- Type 7: Watery with no solid pieces
Gastroenterologists suggest Type 3 or Type 4 is optimal and reflective of a healthier diet and lifestyle, and is easier to pass.
The other five types can signal that something may be off internally. For instance:
- Type 1 and Type 2 stool signals constipation and can be difficult or painful to pass. The most common cause is not enough fluids. Adding fiber to your diet and exercise to your daily routine can also help move things along.
- Type 5 stool can indicate a lack of fiber, which can help soak up fluid and firm things up. Continually pooping in this part of the scale may be a sign of bowel issues.
- Types 6 and 7 are in diarrhea territory and could signal an illness, food poisoning, or some other digestive or intestinal issue. Stress can cause this too. See a doctor if your stool consistently registers on this part of the chart.
Your poop should be a basic brown color. This color comes from the mixing of the various ingredients in your digestive tract, including:
- Bile that breaks down fats passing through the digestive system
- Bilirubin, a substance created when red blood cells reach the end of their life cycle and exit your body as a waste product
- The digested remnants of all the food you ate
Sometimes, poop can be a color other than brown due to something we ate. Vegetables, fruits, and food dyes can change the color of poop, which is perfectly normal.
It is important to know that a food-related tint should disappear within a day or so once the source is out of your system. However, if this color lasts longer than normal, it could be a warning sign of other medical issues. For example:
- Greenish poop could be due to a bacterial or viral infection, a parasite, or irritable bowel syndrome. It can also be connected to new medications you’re taking
- Reddish poop could indicate rectal bleeding or conditions such as hemorrhoids, anal fissures, inflammatory bowel disease, ulcers, or even colorectal cancer
- Blackish poop could signal that there is blood in the upper digestive system from ulcers. It may also be a byproduct of taking iron supplements
- Yellowish or greyish poop could signal liver, gallbladder, or pancreas disorders
Contact a healthcare provider if your poop lingers on the wrong part of the color chart for more than a few days.
Poop smells bad. However, some poop can smell worse than others. Foul-smelling poop is often connected to unwanted bacteria living in your gut, disrupting your usual digestive process.
Symptoms should clear up quickly if the smell is because of something you ate. Speak to a healthcare provider if the issue lasts longer than normal to see if there could be an underlying medical condition that is causing the smell.
Staying aware of the size, shape, color, and smell of your poop is good to do, but not necessary to do every day. If something is wrong with your digestive system, you will know.
If you would like to speak with a gastroenterologist at Jamaica Hospital Medical Center’s Ambulatory Care Center, please call (718) 206-7001 to schedule an appointment.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.
 August 31st is International Overdose Awareness Day. It is the world’s largest annual campaign to end overdose, remember those we have lost to an overdose, acknowledge the grief of the family and friends left behind, and renew our commitment to end overdose and related harms.
August 31st is International Overdose Awareness Day. It is the world’s largest annual campaign to end overdose, remember those we have lost to an overdose, acknowledge the grief of the family and friends left behind, and renew our commitment to end overdose and related harms.
 Follow
Follow