May is Cystic Fibrosis Awareness Month. It is observed as a month that encourages education about the battle against the disease, which affects more than 30,000 people in the United States.
May is Cystic Fibrosis Awareness Month. It is observed as a month that encourages education about the battle against the disease, which affects more than 30,000 people in the United States.
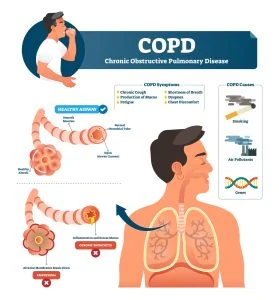
Cystic Fibrosis is a genetic disorder that affects the lungs, causing constant lung infections. It also impacts other organs in the body where mucus builds up, such as the pancreas.
There are two types of cystic fibrosis, classic cystic fibrosis and atypical cystic fibrosis.
Classic cystic fibrosis often affects multiple organs. It is usually diagnosed in the first few years of life.
Symptoms of classic cystic fibrosis include:
- Frequent lung infections
- Loose or oily poop
- Trouble breathing
- Frequent wheezing
- Frequent sinus infections
- A nagging cough
- Slow growth
- Failure to thrive (inability to gain weight despite having a good appetite and taking in enough calories)
Atypical cystic fibrosis is a milder form of the disease. It may only affect one organ, or symptoms may come and go. It is usually diagnosed in older children or adults.
People with atypical cystic fibrosis may have some of the same symptoms as those with classic cystic fibrosis. Over time, they might experience symptoms that can include:
- Chronic sinusitis
- Nasal polyps
- Dehydration or heatstroke from abnormal electrolyte levels
- Diarrhea
- Pancreatitis
- Unintended weight loss
Changes to the cystic fibrosis transmembrane conductance regulator (CFTR) gene cause cystic fibrosis. It affects the cells that make mucus, sweat, and digestive juices. When the CFTR protein doesn’t work as it should, it results in a thick, sticky mucus in the respiratory, digestive, and reproductive systems, as well as extra salt in sweat.
Changes in the CFTR gene that cause cystic fibrosis are divided into several different groups based on the problems they cause. Different groups of gene changes affect how much CFTR protein is made and how well it works.
To have cystic fibrosis, children must get one copy of the changed CFTR gene from each parent. If children get only one copy, they won’t develop cystic fibrosis. But they will be carriers and could pass the changed gene to their children. People who are carriers may have no symptoms of cystic fibrosis or a few mild symptoms.
Because cystic fibrosis is a genetic condition, family history is a risk factor. Cystic fibrosis occurs in all races. However, it is most common in white people of North European ancestry. Because it is less common in people who are Black, Hispanic, Middle Eastern, Native American, or Asian, this may lead to a much later diagnosis.
A late diagnosis may cause worse health issues. Early and effective treatment can improve your quality of life, prevent complications, and help you live longer. If you are a person of color and have symptoms that could be cystic fibrosis, talk to your healthcare provider so you can get tested for it.
To diagnose cystic fibrosis, healthcare providers usually perform a physical exam, review your symptoms, and perform tests.
Every state in the U.S. now routinely screens newborns for cystic fibrosis. Early diagnosis means treatment can begin right away. Testing can include:
- Newborn screening
- A sweat test
- Genetic testing
Cystic fibrosis tests may be recommended for older children and adults who weren’t screened at birth. A healthcare provider may suggest genetic and sweat tests if you have repeated bouts of symptoms of cystic fibrosis.
Unfortunately, there is no cure for cystic fibrosis, however, treatment can ease symptoms, lessen complications, and improve quality of life. Close monitoring and early, aggressive intervention are recommended to slow the worsening of cystic fibrosis over time, which can lead to a longer life.
The goals of treatment include:
- Preventing and controlling infections that occur in the lungs
- Removing and loosening mucus from the lungs
- Treating and preventing intestinal blockages
- Getting enough nutrition
To learn more about cystic fibrosis or to make an appointment with a pulmonologist at Jamaica Hospital Medical Center, please call (718) 206-7126.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow