American Diabetes Alert Day is observed each year on the fourth Tuesday in March. The observance was created by the American Diabetes Association to raise awareness of the seriousness of diabetes and highlight the importance of understanding your risk.
American Diabetes Alert Day is observed each year on the fourth Tuesday in March. The observance was created by the American Diabetes Association to raise awareness of the seriousness of diabetes and highlight the importance of understanding your risk.
According to the Centers for Disease Control and Prevention (CDC), diabetes is the seventh leading cause of death in the United States. Furthermore, the CDC reports that, “More than 40 million Americans have diabetes, and more than 1 in 4 adults with diabetes don’t know they have it.”
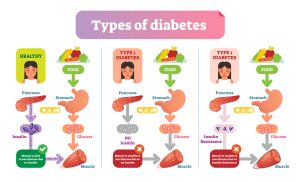
Diabetes is a chronic disease that occurs when blood glucose (or blood sugar) levels are too high. This happens because the pancreas does not produce enough insulin to help regulate the amount of sugar that enters the body’s cells. As a result, excess sugar accumulates in the bloodstream.
If diabetes is not managed properly or is left untreated, it can lead to complications and increase the risk of serious health problems. Diabetes complications include:
- Damage to the nerves in the body
- Kidney problems
- Skin problems
- Bladder problems
- Eye diseases that can lead to blindness
- Gum disease
- Foot complications that can lead to limb loss
- Cardiovascular disease, potentially increasing the risk of hypertension, heart attack, or stroke
Some people are more at risk of developing diabetes than others. You may have an increased risk if you:
- Are overweight or obese
- Are physically inactive
- Have non-alcoholic fatty liver disease
- Have a parent or sibling with diabetes
- Have ever had gestational diabetes
- Are age 45 and older
- Are a Hispanic or Latino, African American, American Indian, or Alaska Native person. (The CDC states that some Pacific Islander and Asian American people also have a higher risk.)
Diabetes Alert Day serves as a “wake up call” to pay attention to these risk factors and properly manage your health. If you are at risk of developing diabetes, you should speak with your doctor about ways to improve your health and lower the chances of complications occurring. To schedule an appointment with a doctor at Jamaica Hospital Medical Center, please call 718-206-7001.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow