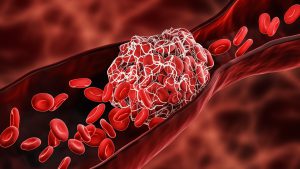
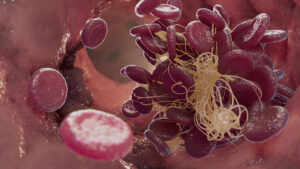
 Blood clots are gel-like clumps of blood that have partially solidified in a blood vessel. Clotting is a natural and essential process that stops bleeding when you’re injured. However, some blood clots can form anywhere along the 60,000 miles of blood vessels in the body and are most likely to happen in the veins. These are called venous blood clots. The most common kinds of venous blood clots are:
Blood clots are gel-like clumps of blood that have partially solidified in a blood vessel. Clotting is a natural and essential process that stops bleeding when you’re injured. However, some blood clots can form anywhere along the 60,000 miles of blood vessels in the body and are most likely to happen in the veins. These are called venous blood clots. The most common kinds of venous blood clots are:
- Deep vein thrombosis (DVT)- DVT usually forms in the legs in the deep veins of the body. Thrombosis is when clots stay put and block blood flow.
- Pulmonary embolism (PE)- Embolisms are blood clots that break free and travel to other parts of the body. If a DVT breaks off and travels to the lungs, it can create a pulmonary embolism.
Arterial clots are less common, occurring when a blood clot clogs an artery. These clots can block oxygen from reaching the heart or brain, which can lead to a heart attack or stroke.
Anyone can develop a blood clot; however, certain factors can increase the risk of developing them, including:
- Prolonged immobility, such as during long flights or hospital stays
- Surgery, especially involving the legs, hips, or abdomen
- Pregnancy and the postpartum period
- Hormonal birth control or hormone replacement therapy
- Smoking
- Obesity
- Family history of blood clots or clotting disorders
- Cancer or cancer treatments
- Age
Recognizing the signs and symptoms of a blood clot can be lifesaving. Here are the signs and symptoms to watch out for:
- Swelling in one limb
- Pain or tenderness in the affected area
- Red or discolored skin
- Warmth in the skin
- Sudden shortness of breath
- Chest pain
- Coughing, possibly with blood
- Rapid heartbeat or palpitations
- Leg fatigue or heaviness
- Dizziness or fainting
Blood clots are known to be silent killers as their symptoms can be similar to symptoms of other, less serious conditions. That’s why it is crucial to understand and recognize the signs and symptoms of blood clots, especially if you are at an increased risk of developing them. Awareness and timely action can help prevent major complications from a stroke, pulmonary embolism, or heart attack.
If you are experiencing symptoms of a blood clot or think you may be at risk of developing one, you can schedule an appointment with one of our vascular surgeons in NYC or learn more about the services at our vascular surgery center in New York. Please call 718-206-6713.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow