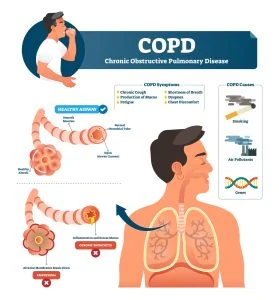
 Chronic obstructive pulmonary disease, or COPD, is a group of health conditions, such as chronic bronchitis and emphysema, that limit airflow in the lungs.
Chronic obstructive pulmonary disease, or COPD, is a group of health conditions, such as chronic bronchitis and emphysema, that limit airflow in the lungs.
Many myths and misconceptions exist about COPD. Here are some misconceptions surrounding COPD:
Myth #1: Only people who smoke get COPD
COPD is often associated with smoking, as smoking cigarettes and other tobacco products is the most common cause of the damage done to the lungs and airways. However, nearly 30% of people with COPD have never smoked a cigarette. Nonsmoking causes of COPD include:
- Long-term exposure to polluted air, such as smog in an urban area or dust and fumes at a workplace
- Genetics plays a role, specifically a condition called Alpha-1 antitrypsin deficiency (Alpha-1)
- Asthma that’s active or even inactive. Researchers have found that 29% of people with asthma eventually receive a COPD diagnosis
- Childhood respiratory illnesses, such as pneumonia
Myth #2: COPD is rare
According to estimates from the Centers for Disease Control and Prevention (CDC), over six in 100 adults in the U.S. had a COPD diagnosis in 2022.
That means millions of adults across the country have received a diagnosis of COPD. The actual proportion of adults with COPD may be higher due to delays in obtaining a diagnosis.
Myth #3: Exercise is too hard if you have COPD
Shortness of breath, wheezing, a chronic cough, and fatigue can all be a part of COPD. Any one of these symptoms can make exercising challenging.
Moderate exercise may not affect your lungs. In some cases, exercise can minimize the symptoms of COPD while strengthening the heart and helping reduce stress.
Try to build up to 20 to 30 minutes of exercise three to four times a week. Combine safe cardiovascular activities such as walking or biking with stretching and strength-building. It won’t be easy to start exercising. Speak with your healthcare provider about building an exercise plan that works for you. They may be able to connect you with a respiratory therapist for breathing techniques and exercises you can do. It is recommended that you speak to your doctor about your health before starting a new exercise regimen.
Myth #4: Only older people develop COPD
COPD is more common in people 65 or older. However, younger people can also develop this condition.
A 2023 study found that COPD affected more than 1.6% of adults ages 20 to 50 in the U.S. Adults aged 35 to 50 had a higher risk of COPD than those under the age of 35.
A history of smoking or secondhand smoke exposure significantly increases the risk of COPD in young adults.
Myth #5: COPD is a man’s disease
The Centers for Disease Control (CDC) reports that women are more likely to develop COPD than men in the U.S.
More women than men have also died from COPD since 2000 in the U.S.
Exposure to tobacco smoke and other pollutants raises the risk of COPD for anyone; however, women can experience more harmful effects than men from these pollutants.
Women with COPD also tend to get a diagnosis later than men, after the disease has progressed and treatment is less effective. This may contribute to reduced survival in women with COPD.
Myth #6: Nothing can be done to treat COPD
COPD treatments are available to help limit symptoms and potentially slow the progression of COPD.
Your treatment plan can include lifestyle changes like quitting smoking (if you smoke), as well as one or more of the following:
- Vaccinations
- Medications
- Pulmonary rehabilitation
- Supplemental oxygen
- Lung transplant
- Surgery
Talk with your healthcare provider to learn more about your treatment options.
Myth #7: There’s no point in quitting smoking after you develop COPD
Avoiding tobacco smoke is one of the most important things you can do to manage COPD.
If you smoke, cutting back and quitting can help limit symptoms and slow the progression of COPD.
Although more research is necessary, it may also be helpful to avoid e-cigarettes and other vaping products.
Avoiding smoking and vaping altogether is likely your healthiest option. Talk with a healthcare provider to learn about smoking cessation counseling, medication, or other resources that can help you cut back and quit smoking or vaping.
Jamaica Hospital’s Medical Home Department has partnered with the American Lung Association to bring you Freedom from Smoking, a comprehensive and successful group-based smoking cessation program. For more information or to register, call: 718-206-8494
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow

