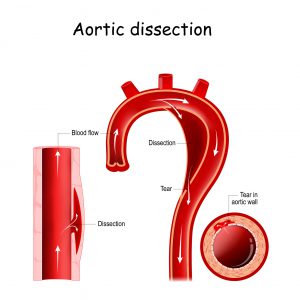
 An aortic dissection is a serious condition that occurs when blood rushes through a tear in a weakened area of the aorta’s wall causing it to split or dissect.
An aortic dissection is a serious condition that occurs when blood rushes through a tear in a weakened area of the aorta’s wall causing it to split or dissect.
Symptoms of aortic dissection can be similar to the symptoms of other heart problems like a heart attack. These signs and symptoms include:
- Sudden severe chest or upper back pain.
- Sudden severe stomach pain.
- Loss of consciousness.
- Shortness of breath.
- Symptoms that are similar to those of a stroke.
- Weak pulse in one arm or thigh.
- Leg pain
- Difficulty walking
Aortic dissections are divided into two groups, depending on which part of the aorta is affected. These groups are:
- Type A- is more common and dangerous. It involves a tear in the part of the aorta where it exits the heart. A tear may also occur in the upper aorta.
- Type B- involves a tear in the lower aorta only.
Some factors that can raise your risk of aortic dissection include:
- Hypertension
- Hardening of the arteries
- Aortic aneurysm
- An aortic valve defect
- A narrowing of the aorta at birth
Certain genetic diseases can also increase the risk of aortic dissection. They include:
- Turner syndrome
- Marfan syndrome
- Other connective tissue disorders.
- Inflammation of the arteries
Other potential risk factors for aortic dissection include:
- Sex
- Age
- Pregnancy
- Cocaine use
- High-intensity weightlifting.
Aortic dissection is uncommon and usually occurs in men in their 60s and 70s. The condition can cause many complications including:
- Death due to severe internal bleeding.
- Organ damage, such as kidney failure or life-threatening intestinal damage.
- Stroke
- Aortic valve damage or rupture into the lining around the heart.
It can be challenging to detect an aortic dissection because symptoms can mimic those of other diseases and health problems which can delay a diagnosis.
A doctor may think you have aortic dissection if you have:
- Sudden tearing or ripping chest pain.
- A difference in blood pressure between the right and left arms.
- Widening of the aorta on a chest X-ray.
Tests to diagnose aortic dissection include:
- Transesophageal echocardiogram (TEE)
- CT scan of the chest.
- MRA
An aortic dissection is a medical emergency that requires immediate treatment. Treatment can include surgery or medications depending on the area of the aorta involved.
Treatments for Type A and Type B aortic dissection may include:
- Surgery
- Medications
After treatment, you may need to take medication to control your blood pressure for the rest of your life. You may also need regular CT or MRI scans to monitor your condition.
If you are experiencing any symptoms of aortic dissection, you can schedule an appointment at Jamaica Hospital Medical Center’s Cardiology Department by calling (718) 206-7100. If you are experiencing an emergency, please dial 911 right away.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow






 The MediSys Health Network (Comprised of Jamaica Hospital Medical Center and Flushing Hospital Medical Center) is pleased to announce the launch of its new application and comprehensive patient platform, MediSys Connect.
The MediSys Health Network (Comprised of Jamaica Hospital Medical Center and Flushing Hospital Medical Center) is pleased to announce the launch of its new application and comprehensive patient platform, MediSys Connect.

