 Chronic migraines are a severe, recurring type of headache that is often debilitating. Migraines have four phases, which are prodrome, aura, migraine headache, and postdrome.
Chronic migraines are a severe, recurring type of headache that is often debilitating. Migraines have four phases, which are prodrome, aura, migraine headache, and postdrome.
Although the exact cause of migraines is unknown, researchers believe genetics is a factor.
There are a few conditions and lifestyle factors that can trigger a migraine, including:
- Anxiety
- Bipolar disorder
- Depression
- Epilepsy
- Sleep disorders
- Caffeine or withdrawal from caffeine
- Taking certain medications or taking them too often
Migraines are more likely to occur in the morning, making it common to wake up with a migraine. Some people have a predictable pattern of migraines, such as just before a menstrual period. Other people may have trouble recognizing what triggers their migraines.
There is no cure for migraines, but they can be managed and prevented with over-the-counter triptans and pain relievers.
Another treatment that can be used for chronic migraines is Botox. Botox for migraines is a type of botulinum toxin that may prevent chronic migraines and is only recommended by a healthcare provider if a person has 15 or more headaches per month.
Although Botox is mostly known for its cosmetic use, it has medical benefits, such as blocking pain signals before they reach the brain, as certain nerves are highly active during a migraine.
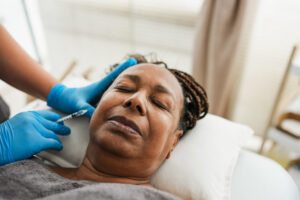
To prevent this from happening, a healthcare provider injects Botox into specific muscles in the head, neck, and shoulders using a tiny needle. These areas connect to the nerves that send pain signals during a migraine. Botox travels along these connected nerves towards the brainstem and blocks the release of chemicals that trigger pain. This may reduce how often a person gets a migraine or make their symptoms less severe when they experience one.
Before receiving Botox for migraine treatment, you will meet with your healthcare provider, who will explain the risks and benefits of it and make sure that it is a safe option for you. If you agree to move forward, you will sign a consent form.
It is important to let your healthcare provider know about any medications and supplements that you are currently taking, as Botox may interact with different types, such as muscle relaxants.
Botox has many side effects, including:
- Mild pain and bruising at the injection site
- Neck pain and stiffness
- Headache
- Flu-like symptoms
- Temporary changes in appearance
These side effects are usually minimal and will clear up. Let your healthcare provider know if you are experiencing any severe pain or discomfort.
The main benefits of Botox for migraines are that it reduces:
- The severity of migraines
- The frequency of migraines
- The duration of migraines
Botox for migraines has other benefits, including:
- It’s effective with long-term use and has minimal complications
- It can be combined with other migraine medications
- The side effects may be better tolerated than other medications available
Chronic migraines can be painful and debilitating, and trying to find the right treatment to provide relief can be difficult and frustrating. If you are suffering from chronic migraines and haven’t found the right treatment options to relieve your symptoms, discuss Botox treatment for migraines with your healthcare provider.
If you are experiencing any symptoms of chronic migraines and are interested in Botox for migraines, you can consult with a neurologist at Jamaica Hospital Medical Center. To schedule an appointment, please call (718) 206-7246.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow