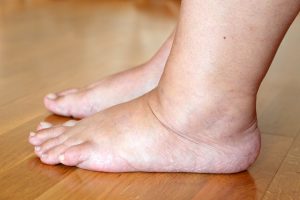
 Water retention or edema occurs when fluid builds up in your tissues, often in your feet, legs, and ankles. It can also affect other body parts such as your face, hands, and abdomen. Edema can affect anyone, especially people who are pregnant and adults 65 and older.
Water retention or edema occurs when fluid builds up in your tissues, often in your feet, legs, and ankles. It can also affect other body parts such as your face, hands, and abdomen. Edema can affect anyone, especially people who are pregnant and adults 65 and older.
Symptoms of edema include:
- An area of your body is larger than it was the day before
- The skin over the swollen area looks stretched and shiny
- Difficulty walking if your legs, ankles, and feet swell
- You have a cough or trouble breathing
- You feel fullness or tightness in the swollen body part
- You feel mild pain or a sore feeling in the affected area
- Stiff joints
- Weight fluctuations
- Puffiness of the abdomen, face, and hips
- Bloating
There are many causes associated with edema, including:
- Standing or sitting for too long
- Weakened valves
- Underlying medical conditions
- Side effects from medication
- Poor nutrition
- Pregnancy
- Compromised immune system
Your healthcare provider will perform a physical examination to diagnose edema, followed by diagnostic tests to find the cause. They will look for swelling, especially on parts of your body where your skin has a shiny, stretched appearance.
Edema grading is a scale used to identify the severity of your edema diagnosis and estimate how much fluid built up in your tissues.
Treatment for edema varies based on the cause, especially if the cause relates to an underlying health condition. Examples of this include:
- If lung disease causes edema, such as emphysema or chronic bronchitis, your healthcare provider will recommend you quit smoking.
- If edema occurs with chronic heart failure, your healthcare provider will recommend lifestyle changes to treat your diagnosis by monitoring your weight, fluid intake, and salt intake. They may also recommend cutting back on the amount of alcohol you drink.
- If edema is a side effect of a medication you are taking, your healthcare provider may stop or lower the dosage of your medication to resolve swelling. Do not stop taking your medication unless your healthcare provider tells you to.
There are a few steps you can take to keep fluid from building up in your body, including:
- Keeping your legs elevated above the level of your heart when you are sitting or lying down.
- Avoid sitting or standing for long periods without moving or going on short walks.
- Wearing support socks, stockings, or sleeves, that put pressure on body parts to keep fluids from collecting there.
- Reducing the amount of salt in your diet.
- Following your doctor’s directions for taking medications. Your doctor may want you to take a diuretic to help you get rid of excess fluid.
If you are experiencing swollen legs, ankles, or feet, you can schedule an appointment with a doctor at Jamaica Hospital Medical Center by calling 718-206-7001.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow