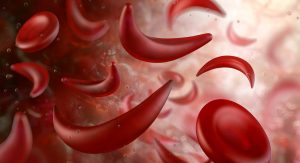
 Sickle cell disease is a group of inherited blood cell disorders that affect hemoglobin, the protein that carries oxygen through the body. A genetic mutation in the HBB gene causes sickle cell disease. The HBB gene is responsible for making a part of hemoglobin. The disease gets its name from the abnormal crescent or “sickle” shape that some red blood cells develop, causing those red blood cells to block the blood flow through the body, creating recurring episodes of pain.
Sickle cell disease is a group of inherited blood cell disorders that affect hemoglobin, the protein that carries oxygen through the body. A genetic mutation in the HBB gene causes sickle cell disease. The HBB gene is responsible for making a part of hemoglobin. The disease gets its name from the abnormal crescent or “sickle” shape that some red blood cells develop, causing those red blood cells to block the blood flow through the body, creating recurring episodes of pain.
Sickle cell disease is a lifelong disease affecting more than 100,000 people in the United States and 20 million worldwide. It is the most common inherited blood disorder in the United States. In the U.S., most people who have sickle cell disease are of African ancestry or identify themselves as black. About one in 13 Black or African American babies is born with the sickle cell trait. About one in every 365 Black or African American babies is born with sickle cell disease. Many people who come from Hispanic, Southern European, Middle Eastern, or Asian Indian backgrounds also have sickle cell disease.
There are many symptoms of sickle cell disease. Early symptoms can include:
- Jaundice- a condition that causes the color of the skin or whites of the eyes to turn yellow
- Extreme tiredness
- Painful swelling of the hands and feet
Many serious symptoms and complications of sickle cell disease include:
- Episodes of severe pain
- Anemia symptoms- fatigue, shortness of breath, dizziness, and an irregular heartbeat
- Fever
- Acute chest syndrome
- Stroke
- Priapism
- Avascular necrosis
- Pulmonary hypertension
- Organ damage
- Leg ulcers
- Gallstones
- Deep vein thrombosis
- Pregnancy complications
- Vision problems
- Frequent infections
Sickle cell disease is diagnosed using a blood test that can check for the form of hemoglobin that underlies sickle cell anemia. In the United States, this test is part of routine newborn screening, but older children and adults can also get it.
If you or your child has sickle cell disease, your healthcare provider may suggest other tests to check for possible complications. If you or your child carries the sickle cell gene, you will likely be referred to a genetic counselor.
If you have sickle cell disease, there are many ways to manage and treat it, including:
- Medicines
- Blood transfusions
- Blood and bone marrow transplant
- Gene therapies
- Complementary and alternative medicine (CAM)
Your healthcare team will probably include a doctor specializing in blood diseases called a hematologist.
If you need help managing symptoms of sickle cell disease or sickle cell trait, schedule an appointment with a hematologist at Jamaica Hospital Medical Center’s Department of Internal Medicine at (718) 206-7001.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow







