 Sleep apnea is a common and potentially serious breathing disorder that causes breathing to stop and restart several times during sleep. These involuntary breathing pauses are called apneic events.
Sleep apnea is a common and potentially serious breathing disorder that causes breathing to stop and restart several times during sleep. These involuntary breathing pauses are called apneic events.
Sleep apnea happens when there is a blockage of the airway or when the brain fails to regulate breathing. This can prevent your body from getting adequate oxygen and lead to various health problems, including:
- High blood pressure
- Increased risk of heart attack, arrhythmia, and other cardiovascular problems
- Increased risk of diabetes
- Sleep deprivation
Common symptoms of sleep apnea include:
- Loud snoring
- Gasping or choking for air during sleep
- Restless sleep
- Breathing pauses
- Daytime fatigue
- Trouble staying asleep
- Hypersomnia (excessive daytime sleepiness)
- Dry mouth
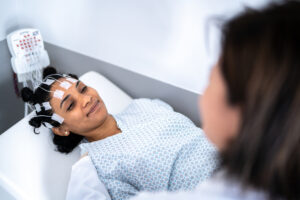
Sleep apnea is diagnosed by a healthcare professional who may ask you about your symptoms, medical history, and sleep history. They may refer you to a sleep specialist or a sleep center to undergo testing. The most common tests for sleep apnea are:
- Polysomnogram, an overnight sleep study conducted in a sleep lab. Here you will be hooked up to equipment that monitors your heart rate, breathing, arm and leg movements, and other functions
- Home sleep apnea test, which is the at-home version of the sleep study. Key metrics and functions are measured with a portable device. Home sleep apnea tests may sometimes miss certain metrics. Therefore, your healthcare provider may still recommend a polysomnogram.
Once diagnosed with sleep apnea, your healthcare provider will recommend treatment based on the severity of your symptoms, general health, and age. Treatment may include lifestyle modifications, oxygen, devices such as a CPAP machine, dental appliances, orofacial therapy, or surgery.
Jamaica Hospital Medical Center’s Department of Sleep Medicine utilizes state-of-the-art technology to diagnose sleep disorders. Several testing options are available at our sleep lab in Queens. We also offer home sleep studies to diagnose obstructive sleep apnea and several treatment devices and therapies, including Inspire Therapy. To schedule an appointment with a sleep specialist, please call 718-206-5916.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow