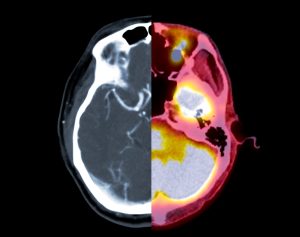
 Chronic traumatic encephalopathy (CTE) is a degenerative brain condition that happens after repeated head injuries. CTE usually affects athletes who play contact sports or military personnel.
Chronic traumatic encephalopathy (CTE) is a degenerative brain condition that happens after repeated head injuries. CTE usually affects athletes who play contact sports or military personnel.
CTE causes neurodegeneration, which means it permanently destroys nerve cells in your brain. Over time, this damage can cause changes in your behavior and mental abilities. It has been associated with second impact syndrome, when a second head injury occurs before symptoms of a previous head injury have fully resolved.
Experts are still trying to understand how repeated head injuries and other factors might contribute to the changes in the brain that result in CTE. Researchers are looking at how the number of head injuries someone experiences and how bad the injuries are may affect the risk of CTE.
There are no specific symptoms that have been linked to CTE, as it shares symptoms with other brain conditions that cause neurodegeneration. It can affect your:
- Cognitive function, which can cause:
- Memory loss
- Trouble solving problems or making plans
- Trouble making a choice or judging what you should do next
- Mild cognitive impairment
- Mood and personality, which can cause:
- Anxiety
- Depression
- Mood swings, especially acting or feeling more aggressive or impulsive
- Personality changes
- Thoughts of self-harm, suicide, or suicidal behavior
- Motor function, which can cause:
- Balance issues
- Loss of coordination
- Tremors, twitches, or other muscle movements you can’t control
There is no way to diagnose CTE in a living person. The only way healthcare providers can confirm CTE is by examining samples of a person’s brain with a microscope during their autopsy.
Even though a healthcare provider may not be able to definitively diagnose CTE while a person is alive, they can still make an educated assumption by building a diagnosis using a few factors, including:
- A physical exam
- A neurological exam
- The symptoms a person is experiencing
- A person’s medical history, especially if they have had head injuries
Experiencing CTE symptoms doesn’t automatically mean a person has it. There are a lot of conditions that can cause similar symptoms. A healthcare provider will use tests to help diagnose or rule out these other issues. Tests include:
- Blood tests
- CT scan
- Lumbar puncture
- MRI
- PET scan
There is no treatment for CTE because there is currently no cure for it. Unfortunately, if a person has CTE, their symptoms will continue to get worse. Avoiding head injuries is the only way to lower your risk of developing CTE. Wear the right protective equipment for all activities and sports, especially helmets or protective headwear.
If you are experiencing any symptoms of CTE, you can schedule an appointment with a doctor at Jamaica Hospital Medical Center’s Ambulatory Care Center by calling (718) 206-7001. If you are experiencing an emergency, call 911.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.

 Follow
Follow






